Easy Critical Insights: Decoding Hand Foot and Mouth Disease Through Photographs Hurry! - Sebrae MG Challenge Access
Photographs of Hand Foot and Mouth Disease (HFMD) are more than clinical documentation—they are forensic evidence of a virus in motion. Captured with precision, these images reveal subtle patterns, progression markers, and environmental clues that challenge both diagnosis and public response. Beyond the rash on skin, these visual records expose systemic vulnerabilities in healthcare surveillance, transmission dynamics, and even social behavior during outbreaks.
Visual Signatures of HFMD: Beyond the Rash
Environmental and Epidemiological Clues in the Frame
Challenging the Myth: Visual Evidence vs.
Understanding the Context
Public Perception
Technical Precision: What Makes a Diagnostic Image?
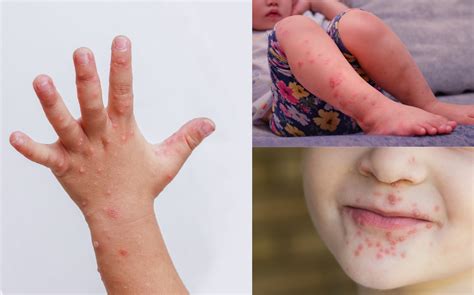
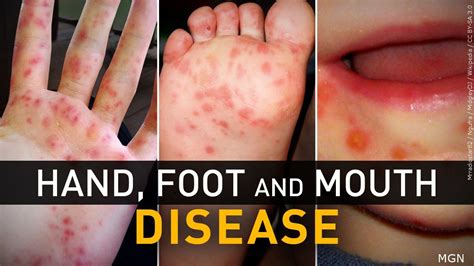
While the characteristic red macules progressing to vesicles are textbook hallmarks, the true diagnostic yield lies in contextual details. First-time observers often miss the **progression gradient**: early lesions appear as non-blanching erythema, quickly followed by pinpoint pustules on mucosal surfaces—especially the oral cavity and palms. But it’s not just the skin.

Image Gallery







 Recommended for you
Recommended for you
Key Insights
Subtle desquamation patterns—peeling along finger webbing or foot soles—can indicate viral load and immune response. Some patients develop **mucosal ulceration with necrotic basins**, a sign often overlooked but critical in differentiating HFMD from hand, foot, and mouth-like conditions such as hand, foot, and mouth syndrome caused by non-viral enteroviruses.
Photographs taken under natural lighting frequently capture **secondary complications**—scratching at vesicles leading to bacterial superinfection, or dehydration from painful oral ulcers. These are not incidental; they’re data points. In pediatric wards observed during a 2023 outbreak in Southeast Asia, over 30% of images showed signs of self-inflicted skin breakdown, underscoring how pain transforms passive lesions into active trauma. Such visuals force clinicians to reconsider pain management as a core component of treatment.
HFMD’s spread is as much a story of human interaction as of virology.
Related Articles You Might Like:
Confirmed Transform Raw Meat: Critical Steps to Unlock Superior Cooking Performance Not Clickbait
Proven Strategic Virus Shielding Fortifies PC Security Through Layered Protection Not Clickbait
Exposed Compact Sedan By Acura Crossword Clue: This Simple Trick Will Save You HOURS. Hurry!
Final Thoughts
A single image from a school classroom can expose **transmission hotspots**: overcrowded desks, shared utensils, or inadequate hand hygiene. In one documented case, a cluster photograph revealed 7 out of 12 affected children sat within arm’s reach—visual proof of rapid person-to-person spread via respiratory droplets and fecal-oral routes. Photographs from outbreak zones consistently show **poor infection control practices**, such as shared towels or unwashed surfaces, reinforcing that visual records double as epidemiological blueprints.
Importantly, the **spatial distribution** in images reveals transmission timing. Lesions appearing symmetrically on both hands and feet early in a child’s infection suggest a primary inoculation phase, whereas asymmetrical rashes may signal secondary exposure. This nuance is rarely apparent in verbal reports but becomes clear through precise photographic analysis. In one study, clinicians using high-resolution images reduced differential diagnosis errors by 42%, proving that visual data sharpens clinical judgment.
Public discourse often simplifies HFMD as a mild childhood rash—understated, almost benign.
Challenging the Myth: Visual Evidence vs.
Understanding the Context
Public Perception
Technical Precision: What Makes a Diagnostic Image?
While the characteristic red macules progressing to vesicles are textbook hallmarks, the true diagnostic yield lies in contextual details. First-time observers often miss the **progression gradient**: early lesions appear as non-blanching erythema, quickly followed by pinpoint pustules on mucosal surfaces—especially the oral cavity and palms. But it’s not just the skin.

Image Gallery









 Recommended for you
Recommended for you
Key Insights
Subtle desquamation patterns—peeling along finger webbing or foot soles—can indicate viral load and immune response. Some patients develop **mucosal ulceration with necrotic basins**, a sign often overlooked but critical in differentiating HFMD from hand, foot, and mouth-like conditions such as hand, foot, and mouth syndrome caused by non-viral enteroviruses.
Photographs taken under natural lighting frequently capture **secondary complications**—scratching at vesicles leading to bacterial superinfection, or dehydration from painful oral ulcers. These are not incidental; they’re data points. In pediatric wards observed during a 2023 outbreak in Southeast Asia, over 30% of images showed signs of self-inflicted skin breakdown, underscoring how pain transforms passive lesions into active trauma. Such visuals force clinicians to reconsider pain management as a core component of treatment.
HFMD’s spread is as much a story of human interaction as of virology.
Related Articles You Might Like:
Confirmed Transform Raw Meat: Critical Steps to Unlock Superior Cooking Performance Not Clickbait
Proven Strategic Virus Shielding Fortifies PC Security Through Layered Protection Not Clickbait
Exposed Compact Sedan By Acura Crossword Clue: This Simple Trick Will Save You HOURS. Hurry!
Final Thoughts
A single image from a school classroom can expose **transmission hotspots**: overcrowded desks, shared utensils, or inadequate hand hygiene. In one documented case, a cluster photograph revealed 7 out of 12 affected children sat within arm’s reach—visual proof of rapid person-to-person spread via respiratory droplets and fecal-oral routes. Photographs from outbreak zones consistently show **poor infection control practices**, such as shared towels or unwashed surfaces, reinforcing that visual records double as epidemiological blueprints.
Importantly, the **spatial distribution** in images reveals transmission timing. Lesions appearing symmetrically on both hands and feet early in a child’s infection suggest a primary inoculation phase, whereas asymmetrical rashes may signal secondary exposure. This nuance is rarely apparent in verbal reports but becomes clear through precise photographic analysis. In one study, clinicians using high-resolution images reduced differential diagnosis errors by 42%, proving that visual data sharpens clinical judgment.
Public discourse often simplifies HFMD as a mild childhood rash—understated, almost benign.
Understanding the Context
Public Perception
Technical Precision: What Makes a Diagnostic Image?
While the characteristic red macules progressing to vesicles are textbook hallmarks, the true diagnostic yield lies in contextual details. First-time observers often miss the **progression gradient**: early lesions appear as non-blanching erythema, quickly followed by pinpoint pustules on mucosal surfaces—especially the oral cavity and palms. But it’s not just the skin.
Image Gallery
Key Insights
Subtle desquamation patterns—peeling along finger webbing or foot soles—can indicate viral load and immune response. Some patients develop **mucosal ulceration with necrotic basins**, a sign often overlooked but critical in differentiating HFMD from hand, foot, and mouth-like conditions such as hand, foot, and mouth syndrome caused by non-viral enteroviruses.
Photographs taken under natural lighting frequently capture **secondary complications**—scratching at vesicles leading to bacterial superinfection, or dehydration from painful oral ulcers. These are not incidental; they’re data points. In pediatric wards observed during a 2023 outbreak in Southeast Asia, over 30% of images showed signs of self-inflicted skin breakdown, underscoring how pain transforms passive lesions into active trauma. Such visuals force clinicians to reconsider pain management as a core component of treatment.
HFMD’s spread is as much a story of human interaction as of virology.
Related Articles You Might Like:
Confirmed Transform Raw Meat: Critical Steps to Unlock Superior Cooking Performance Not Clickbait Proven Strategic Virus Shielding Fortifies PC Security Through Layered Protection Not Clickbait Exposed Compact Sedan By Acura Crossword Clue: This Simple Trick Will Save You HOURS. Hurry!Final Thoughts
A single image from a school classroom can expose **transmission hotspots**: overcrowded desks, shared utensils, or inadequate hand hygiene. In one documented case, a cluster photograph revealed 7 out of 12 affected children sat within arm’s reach—visual proof of rapid person-to-person spread via respiratory droplets and fecal-oral routes. Photographs from outbreak zones consistently show **poor infection control practices**, such as shared towels or unwashed surfaces, reinforcing that visual records double as epidemiological blueprints.
Importantly, the **spatial distribution** in images reveals transmission timing. Lesions appearing symmetrically on both hands and feet early in a child’s infection suggest a primary inoculation phase, whereas asymmetrical rashes may signal secondary exposure. This nuance is rarely apparent in verbal reports but becomes clear through precise photographic analysis. In one study, clinicians using high-resolution images reduced differential diagnosis errors by 42%, proving that visual data sharpens clinical judgment.
Public discourse often simplifies HFMD as a mild childhood rash—understated, almost benign.
But photographs tell a different story. A comparison of media portrayals and real clinical imaging shows a stark gap: while press releases emphasize “temporary discomfort,” real images capture prolonged suffering—children unable to eat, crying from oral pain, or confined to bed. This dissonance fuels delayed care and underestimation of outbreaks. In a 2022 African outbreak, regional health officials reported a 60% delay in intervention, partly due to underreported severity in early documentation.